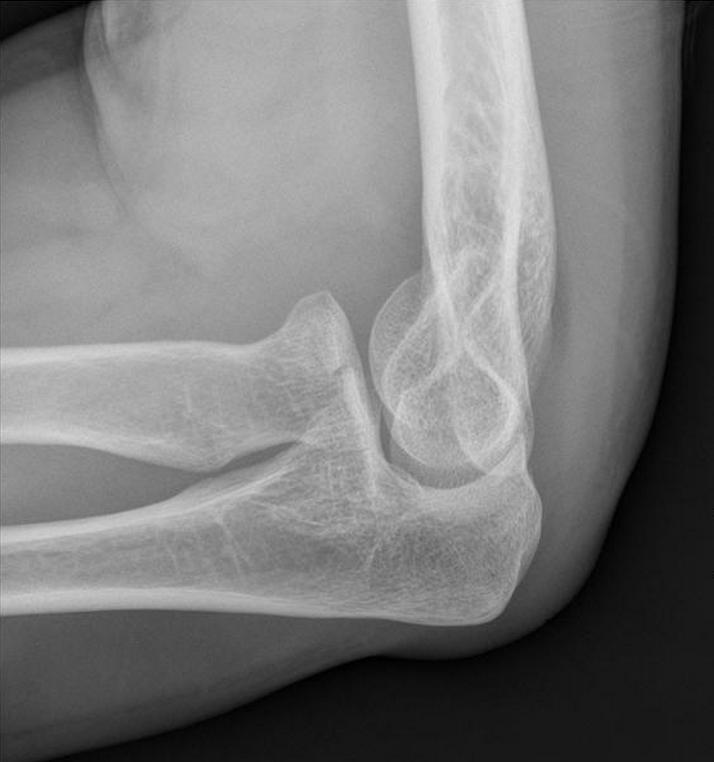 
Seven of these patients reported pain in the region on the distal IOM. In 9 of 14 patients with a Mason type I radial head fracture Hausmann et al found partial lesions of the interosseous membrane (IOM) with MRI. Associated injuries as ligamentous injuries, or bone bruise of the capitellum can be found using magnetic resonance imaging (MRI) in 76% to 96% of the patients with a radial head fracture. Loss of cortical contact and comminution of the radial head fracture are strongly related to a high incidence of associated injuries. van Riet et al found an incidence of associated injures in 39% in a retrospective evaluation of 333 patients with a radial head fracture. When treating patients with a fracture of the radial head, special attention has to be given to the detection and treatment of associated injuries of the injured extremity. Potential benefit of CT reconstructions is to determine the location of the fracture in the radial head (most commonly anterolateral quadrant with the forearm in neutral position), which may be associated with change on associated injuries and elbow instability. Two- or three-dimensional computed tomography (CT) scans improved sensitivity for diagnosis in another study, though the interobserver agreement was still only moderate for most fracture characteristics. The interobserver agreement for diagnosing a 2 mm gap (κ = 0.55) or cortical contact (κ = 0.43) on standard radiographs was moderate. The various classifications are summarized in Table Table1 1 and Figure Figure1. More recently, Rineer et al suggested that the stability of the fracture can be determined based on the detail whether there was cortical contact between the fragments, or not. Subsequently, Broberg and Morrey and Hotchkiss further quantified the amount of dislocation for type II fractures. In 1962, Johnston added fractures of the radial head that were associated with a dislocation of the elbow, as a type IV to the system. Mason Type I fractures (73%) of the radial head involved fractures without displacement, type II fractures (19%) were marginal sector fractures with displacement, and type III fractures (8%) were comminuted. Mason observed, back in 1954, the fracture patterns of the radial head in 100 patients and divided them in three groups. 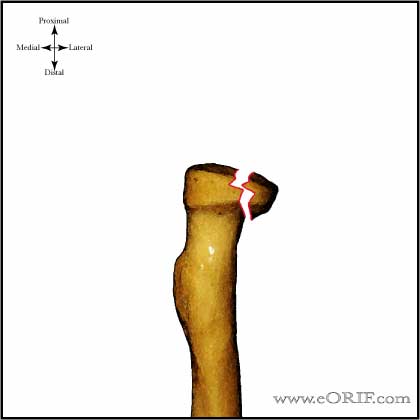
However, the amount of instability was very small, possibly because of the stabilizing effect of the biceps and brachialis. Other studies observed an improved but not normal stability after radial head arthroplasty with MCL insufficiency. Radial head arthroplasty restores valgus stability in elbows with disruption of the MCL to a state similar to that seen in elbows with a native radial head. Pomianowski et al reported that laxity was increased after radial head excision in elbows with disruption of the medial collateral ligament (MCL). These findings suggest that repair of the disrupted LCL complex is essential in order to restore elbow stability following open reduction and internal fixation (ORIF) of the radial head or radial head arthroplasty. Elbow laxity was improved following radial head arthroplasty however, these elbows were still unstable relative to those with intact ligaments. Also an increase in external rotation of the ulna with respect to the humerus during passive motion with the forearm in supination was observed after radial head excision when both ligaments were intact.Ī significant decrease in elbow stability was noted if the radial head was excised in elbows with an associated disruption of the lateral collateral ligament (LCL). Radial head excision alters the kinematics and varus-valgus laxity of the elbow with intact ligaments and that stability is improved after radial head arthroplasty. Several biomechanical studies have been conducted to quantify elbow stability for simulated fractures, radial head excision, and radial head replacement, with and without the integrity of the collateral ligaments. The issue of the individual contributions of the radial head and soft-tissue stabilizers of the elbow is very complex. The radial head is an important secondary stabilizer in valgus and external rotation.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
